Infertility is one of the major problems our readers face, and today gynaecologist and fertility specialist Dr. Neelu Koura talks to us about one of the most common factors – low sperm count. Thankfully, it may be easier to treat than you think.

If you and your partner have been trying to conceive for over six months without any luck, a semen analysis reports is one of the first things a fertility doctor will recommend. Many couples struggling to have a baby encounter the problem of low sperm count or weak sperm in their semen report.
A lot of couples I meet at my fertility clinic, Dr. Neelu Test Tube Baby Centre, are ignorant about the method of getting pregnant that makes them think that female is always the major reason and needs all the tests and treatments.
If there is an issue with the semen, i.e. sperms are low in number, not of good quality or absent completely, we can consider it as the primary reason of the trouble. And this information will help us to decide what investigation is to be done on the female and treatment options, too.
What is Male Factor Infertility?

When a couple is trying to conceive, a good reproductive health of both male and female is necessary. Male contributes his sperm to make a baby. Without the sperm, it is impossible to achieve pregnancy. Male factor infertility means that the reason for the inability to achieve pregnancy by a couple lies in the male and not in the female. This includes any factor which leads to:
- Deterioration of sperm quantity and quality.
- Inability of the sperm to swim up the female tract and reach the egg (motility).
- Sperm’s inability to penetrate the egg.
- Inability of formation of the sperms in testicles of the male.
- Inability to ejaculate these sperm into the female body.
Any of these or a combination of these factors these leads to male factor infertility. And all these can be judged and diagnosed by a simple semen analysis.

Quick Facts
Here are some facts to know about male factor infertility and low sperm count:
1. Male factor infertility accounts for 40% of infertile couples.
2. Bad sperm or even an absence of sperms in a male will only be evident in a semen analysis report.
3. These factors cause no symptoms that may make an individual doubt about it.
4. These are unrelated to the age of the male. A young and healthy male can also be diagnosed to be azoospermic, i.e. no sperm in his semen or testicles. And a 60-70 year old male can have absolutely healthy sperms.
How to Get Semen Analysis Done & What to Expect at the Clinic
Semen analysis should be done at a fertility clinic where there is a facility of a neat and clean private semen collection room. Also it should be done at a clinic where reporting is done by a qualified andrologist. You will be asked to collect your semen sample in a container at the facility, so it is usually recommended to abstain from sexual activity for 2-4 days so that a good sized sample is collected. Abstaining for more than 5 days is not recommended.
What is Sperm & How Does It Contribute to Pregnancy?
A sperm is the male gamete contributed by the father in the process of pregnancy, and which contributes to the paternal DNA of the baby. In simpler words, sperm is a living, motile single celled structure in the semen of a male, which has half the amount of genetic material, i.e. the contribution of the father in the formation of a baby. Sperm are formed in the testicles of the male and are pushed in the semen.
The sperm is a highly energetic cell as it has to perform a tough task. It needs to travel the entire course of the female vagina, enter into the womb, travel the entire distance of around 8-9 cm inside the female’s uterus (womb) . Then it has to find the egg in the fallopian tube of the female.
If it finds the egg – all the sperms that have reached till the egg compete with each other and the best one is able to penetrate the egg. As it penetrates, all the others are expelled automatically away from the egg. This event of penetration of the egg and further steps of forming an initial stage embryo is called fertilization.

What is Considered Unhealthy or Weak Sperm?
World Health Organization (WHO) has laid out the criteria of number, morphology (structure) and motility according to which semen parameters are graded. According to these parameters, we define the sperms to be low in count, poor in quality or motility (weak sperm).
In one ejaculate, more than 1.5 ml of semen is considered normal. Similarly, sperm concentration of more than or equal to 15 million sperms per ml of considered normal. Normally, in 1 ml of semen of a male, there are 80-100-120 million sperm. And a total sperm count of less than 39 million per ejaculate is considered low.
Also their motility and its pattern is important. Immotile sperms are of no use as they cannot swim up to reach the egg. Poorly motile, that is C-grade or D-grade motility sperms will also not be able to reach or penetrate the ovum in the body of a female. Here’s an example of a sperm analysis report where the sperm concentration is normal, but the progressive motility is low.
Their number is an important criteria of normal semen parameter but only the number is not enough. They need to be structurally normal. This means that their parts – head, body and tail – have to be normal. If there is any deformation in any of its parts, it is not considered as healthy enough to be a potential one to penetrate the egg. Here’s an example of how sperm scan looks like:
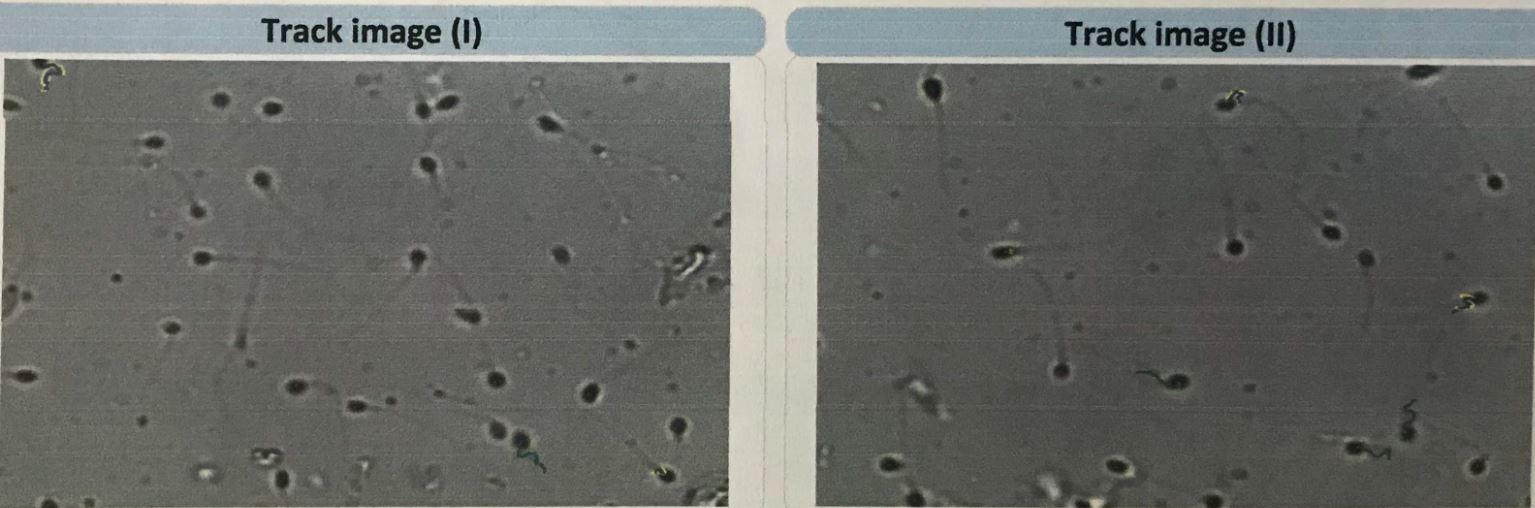
What Causes Weak Sperm & Low Sperm Count?
Both lifestyle and medical factors may contribute to low sperm count or weak sperm. Common causes include obesity, unhealthy diet, smoking, drug use, tobacco and stress. Wearing too tight clothing, heat generated through excessive use of saunas, sitting for extra long periods of time and exposure to harmful toxins or radiations may also cause these issues.
Is It Possible to Have No Sperm?
In some cases, the semen does not have any sperm – that is, nil sperm or Azoospermia. This can happen because of two reasons:
- By birth, the male’s testies cannot form sperms. This is also called Primary Testicular Failure.
- Sperms are being formed but because of obstruction in the duct, they are not being released in the semen. This is also called Obstructive Azoospermia.

People usually get worried when they come to know that there are no sperm, especially if it’s the former case, in which sperms are not being formed in the testies.
I want to clarify that this will only cause trouble in becoming a father. However, it has no effect on your sexual life or general health otherwise. So do not stress.
Now let’s talk about what to do when you encounter any of these issues in your report.
Low Sperm Count Treatment
There are many procedures and treatments your fertility specialist may suggest including:
- Medications to increase sperm count and/or motility
- Intrauterine Insemination (IUI)
- In vitro fertilisation (IVF)
- Intracytoplasmic Sperm Injection (ICSI)
- Donor procedure
- Semen cryopreservation
- Blastocyst culture
Your fertility doctor will suggest these Assisted Reproductive Technology (ART) procedures or treatments depending upon your requirement and situation. Here are some details on different treatments according to your sperm count:
1-10 million/ ml
If your semen analysis report shows a sperm count of 10 million/ml or less, consult an ART (Assisted Reproductive Technology) specialist immediately. Go for fertility treatments of IVF or ICSI at the earliest.
10-30 million/ ml
If your sperm count is between 10 to 30 million/ml, consult an infertility specialist in ART clinic.
- You are recommended to try 3-6 cycles of IUI
- If unsuccessful, shift to IVF or ICSI.
- Try medication for 3 months. Medication will typically be recommended before IUI, depending on your reproductive health.
Weak Sperm Treatment (for Low Motility)
Here are the recommendations if your sperm count is good but your sperm motility is less than normal:
- Stop alcohol consumption.
- Stop smoking.
- Get an examination done by an andrologist.
- Take medication in the form of antioxidants.
- Eat healthy and nutritious meals.
- Try medication for 3-4 months.
- If there is no improvement within 3-4 months after taking the above steps, get an evaluation done in an ART clinic.
- Consider ICSI.
Nil Sperm Treatment
- Testicular biopsy
- For testicular failure, go for IUI with donor sperm, or IVF with donor sperm.
- For obstructive Azoospermia, you are recommended to go for ICSI with TESA (Testicular / Epididymal Sperm Aspiration or Extraction)
Hope this information was helpful to you. If you have further doubts, you can definitely write to me at the email below. Don’t hesitate to write about your experiences in the comments below and I’ll try to read them all.

Dr. Neelu Thapar Koura is a Obstetrician, Gynecologist and General Physician in Moga, Punjab. With an experience of 15 years in these fields, Dr. Neelu Thapar Koura is the Managing Director at Gomti Thapar Hospital, which also houses her fertility and IVF clinic. She did her MBBS from GS Medical College in 1999 and MD – Obstetrics & Gynaecology from Sardar Patel Medical College in 2004. You can find more information about these fertility treatments and Dr. Neelu Test Tube Baby Centre, and contact her by emailing [email protected].